I’ve performed heart surgery on more than 3,230 patients, many of whom suffered from the aftereffects of a heart attack.
So I’m going to tell you the same thing I tell them:
The best thing you can do now is become an active participant in your recovery.
In simpler terms, that means keeping an eye on your metabolic health. You should also keep looking for opportunities to improve your heart health.
Good news: these are things you can do automatically with a continuous glucose monitor.
Here’s what you should know about using CGMs after a heart attack.
A very brief look at CGMs
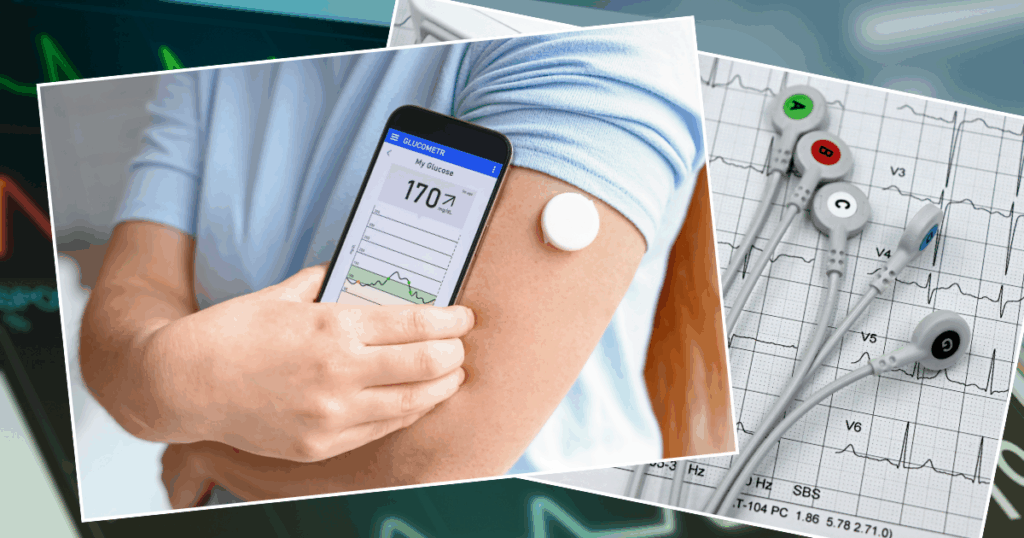
Continuous glucose monitors are wearable health devices that track your blood glucose (blood sugar) throughout the day. Unlike finger-prick tests, which require you to draw blood, CGMs are applied once and then stay on your arm for a period of time, placing a tiny sensor just under your skin to monitor fluctuations.
Of course, that’s not to say wearable health devices are the be-all and end-all of metabolic health metrics. There are gaps left behind requiring third-party measurements, such as blood labs.
But they’re still a great place to start for your health, especially if you’ve recently suffered a heart attack.
Why does glucose monitoring matter after a heart attack?
Blood sugar and heart health are tied at the hip, so keeping a close eye on your numbers could mean the difference between a long healthspan and a chronic disease.
There are three major reasons to get a CGM after a heart attack:
Monitor your glucose variability
Patients with heart disease regularly report high glucose variability (GV), meaning they experience frequent and severe sugar spikes.
Studies also show that hyperglycaemia (high blood sugar) is found in up to 50% of all patients admitted for myocardial infarction. They also found that in “every 18 mg/dL (1 mmol/L) increase in glucose level above 200 mg/dL, it has been reported a 4% and a 5% increase in hospital mortality risk in patients without and with diabetes, respectively.”
Lowering glucose variability after you’ve experienced a heart attack can help avoid the possibility of a second one in the future. Rather than relying on ‘in the moment’ testing such as finger prick tests, you can get immediate, continuous feedback on your blood sugar.
Avoid inflammatory conditions leading to worsened heart health
You can’t necessarily undo all the effects of a heart attack. However, you can minimize the future damage caused.
Remember: one in five patients who experiences a heart attack will experience another. If you’re readmitted within 90 days, you’ll have a 50% higher chance of dying within the next five years.
A CGM can help you avoid this by keeping you mindful of your glucose levels, which ultimately helps you avoid inflammation. This helps stave away conditions like:
- Dementia
- Diabetes
- Gastrointestinal diseases
It also significantly reduces your risk of a second heart attack.
Reduce your re-hospitalization risk
I mentioned above that one in five patients who experiences a heart attack will experience another. It’s also true that one in four patients diagnosed with heart failure are readmitted to the hospital within 30 days of discharge. With statistics like these, it’s important to control every variable that you can, and that includes blood glucose.
Research shows that diabetes (aka dysregulated blood sugar) can increase your risk of heart failure hospitalization by two-fold. If you’re prediabetic or have hyperinsulinemia, you might be at an extraordinary risk.
The good news is that continuous glucose monitoring can help you better understand blood sugar levels throughout the day, and empower you to make early lifestyle changes.
It’s much easier to engage in proactive healthcare when you have tools that do it for you, after all.
Best practices for using a CGM post-heart attack
To help make the most of the next six to nine months, I suggest taking the following actions:
Identifying your glucotype
I’ve spoken before about lean mass hyper responders, or people who experience extreme changes to their cholesterol in response to low-carb diets. A similar concept can be applied to blood glucose control. These are referred to as glucotypes: unique blood sugar patterns based on individual biology.
There are three to consider:
- Low: Very little blood sugar variation throughout the day
- Moderate: A medium amount of blood sugar variation
- Severe: Significant blood sugar variations
Yes, blood sugar will look different between two people if they follow different diets (say, vegan versus carnivore). But as researchers explain, “the physiology underlying dysglycemia is highly variable between individuals.” Glucotypes help to categorize individuals based on specific patterns of glycemic responses.
Knowing which type of glucotype you are can help you make better decisions about food and exercise. You might not want to eat many, if any, carbohydrates if you know you’re in the ‘severe’ bracket, for example.
And while we’re on the subject of bioindividuality…
Tracking changes according to food and exercise
I’m a big believer in N=1, or that people react differently to the same environmental factors. That means the foods and exercises that work for someone else may or may not have the same impact on your glucose.
Let’s say you eat blueberries along with some scrambled eggs for breakfast. Even though blueberries are categorized as having a low glycemic index, you still notice a sizable impact on your glucose. This may be a sign that you’re more sensitive to the sugar content in fruit.
The same is true for exercise. For example, you might try running and walking to level out your blood sugar, only to be left with middling results. When you start resistance training, you see an enormous benefit. It’s no wonder why: studies show that different physiques respond differently to exercise.
To summarize: CGMs can make your heart attack recovery period more personalized. Just pair data from your CGM with logs of your food and exercise, then determine the best possible plan for your metabolic health.
Pairing CGM data with blood work
I’ve said it before, but it’s worth repeating: wearable devices will only take you so far. The most holistic method of measuring your heart health is always going to include regular blood work.
I recommend starting with:
- Complete blood count (CBC)
- Complete metabolic panel (CMP)
- Advanced lipid testing
- Fasting Insulin level
Now, if you’re following a new diet — say, low-carb, keto, or carnivore — you may notice some numbers look wildly different from before. This is normal and expected (yes, even for your cholesterol).
I cover this more thoroughly in my guide to changing biomarkers on ketogenic diets.
Taking your first few steps
There’s no shame in having experienced a heart attack, but there is great pride in taking the reins of your recovery.
You have the next six months to make the greatest amount of difference. And armed with a CGM, I invite you to read my guide on heart attack recovery.