The American Heart Association (AHA) has been in the news lately, for disagreeing with the US’s new dietary guidelines. In particular, insisting that people should avoid full-fat dairy and get their protein from plants instead of meat.
This creates more confusion for the American public, who are witnessing public disagreement between two groups that give public health advice.
But here’s the thing: we’ve followed the AHA approach for 70 years, and the result is an America that is sicker than ever. A few years ago I wrote an article looking at how the AHA’s 2021 guidelines continued to fail us, but they’re still clinging to and promoting the same advice.
Why is the AHA sticking so heavily to outdated science? And what are the outcomes of following their dietary guidelines compared to the new recommendations?
This article will explore these questions in more detail.
Article overview
- The AHA’s new nutrition guidance recommends plant-based protein and low-fat dairy.
- These suggestions contrast with the new US dietary guidelines for 2026, which recommend larger portions of animal protein and full-fat dairy.
- After following the AHA’s guidelines for years, most Americans have experienced objectively worse heart health outcomes.
- It should also be noted that the AHA accepts research and funding from diametrically opposed organizations.
- The new dietary guidelines have a strong scientific backing, as well as better heart health outcomes, for diet-based chronic diseases.
The AHA’s recommended guidelines for 2026

Before we dive into outcomes here, let me review the important highlights of the AHA’s 2026 guidelines.
Very little has changed from its 2021 public report, which I explain in this article.
Let’s go in order of best to worst suggestions.
- Avoiding added sugars, ultraprocessed foods, and alcohol. Yes, yes, and yes to all of these. Avoiding sodium at all costs isn’t necessarily a ‘must’ for good heart health though, and you can read more about my thoughts on salt and hydration.
- Eating plenty of fruits and vegetables. I have no qualms with this, and neither do the new guidelines. My only note would be to watch your fiber intake if you struggle with chronic disease like IBS. Also, keep an eye on your fruit and blood sugar levels if you’re a type 2 diabetic or are insulin resistant.
- Choosing ‘healthy’ proteins. According to the list, that includes fat-free yogurt, beans, tofu, several other plant-based sources, chicken and fish. There’s no mention of red meat anywhere on the list, and that’s intentional: the AHA has vilified ruminant protein. But considering the very low bioavailability of the plant-based sources, not to mention the problems with low-fat diets and fake meat, there’s very little chance this will be enough for good heart health. I do agree with the suggestions for eating more chicken, milk, tuna, and salmon. But you should keep a watchful eye on things like almonds, which are known to contain high levels of oxalates.
- Eating more unsaturated fats. The new US dietary guidelines recommend butter, beef tallow, and olive oil as fat sources for cooking and baking. Unfortunately, olive oil is just about the only similarity between lists. The AHA recommends seed and vegetable oils such as soybean, canola, and corn. It also recommends avoiding ‘tropical’ oils such as coconut, since it’s high in saturated fat.
- Choosing ‘whole grains.’ Oats, whole wheat pasta, and wheat bread are carbohydrates and contrary to popular belief, you don’t need carbohydrates to support your heart health. In many cases, it can actually harm it. Although they can have their place in a metabolically healthy diet, people with inflammation or insulin resistance should reconsider eating them. But the AHA still continues to promote grains for reducing cholesterol, which has long been the almost singular focus on heart disease prevention.
Why aren’t the AHA’s guidelines making anyone healthier?
If we’re looking at it on a very basic level, the dietary guidelines put forth by the AHA are extremely similar to the new US guidelines. Both encourage eating whole, real foods, avoiding processed foods, and reducing your sugar intake. I don’t have a problem with any of these things.
As one Health and Human Services (HHS) spokesman recently put it: “[dietary guidelines from the department and the AHA are] aligned on the major issues: eat real food, avoid highly processed food, and limit refined grains and added sugar. We look forward to working collaboratively with the AHA to evangelize these core principles and reverse the diet-related chronic disease epidemic.”
The issue here is that the AHA both excludes and promotes things we know to be damaging to metabolic health.
For example, a high carbohydrate diet contributes directly to atherosclerosis and vascular disease. And yet, that’s exactly what the AHA recommends: they support the claim that “45% to 65% of calories should come from carbohydrates.”
Additionally, the encouragement to avoid animal-based protein has very little to do with actual science. Research shows that unprocessed red meat could help feed your gut microbiota. Other studies show that “daily unprocessed beef intake do not significantly affect most blood lipids, apolipoproteins, or blood pressures.”
Dr. Stacey Rosen, the president of AHA, has only commented that “[the government’s encouragement to eat red meat and full-fat dairy products] has been shown repeatedly to be a not healthy way to eat.” She also states that the AHA’s dietary guidelines are “based on decades of science.”
It’s worth pointing out that Americans have followed the AHA’s advice for the past 70 years. We ate high-carb meals, low-fat yogurt, and plenty of unsaturated margarine products. And yet, our hearts are less healthy than they’ve ever been.
Just look at the increase of young people winding up on operating tables across the country. Cardiovascular disease in young adults has almost doubled in the past 15 years.
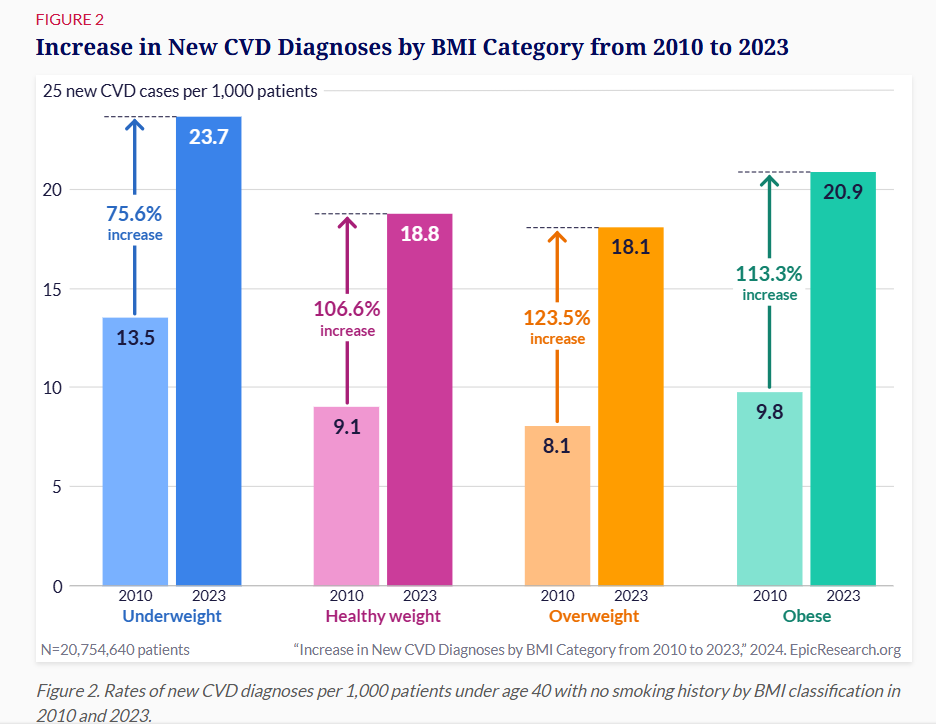
This misguided dietary advice continues to affect the health and wellness of at-risk populations. Case in point: the ADA’s guidelines for type 2 diabetics claimed that up to a fourth of your plate could be a ‘quality carbohydrate choice’ for every meal. Not only will this eating pattern exacerbate the problem (i.e., insulin), but it can potentially make your diabetes worse.
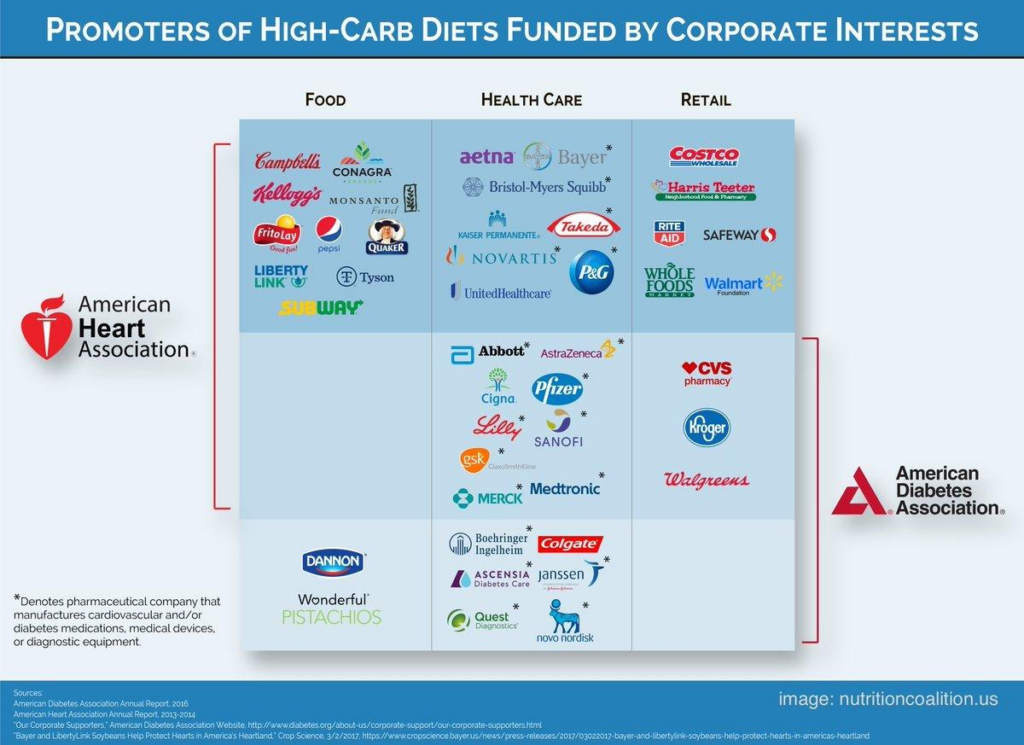
This, unfortunately, shouldn’t be surprising to anyone. The American Heart Association receives massive amounts of funding from companies like Kellogg’s, Quaker, Subway, and others. The ADA, on the other hand, receives money from ultra-processed food companies like Dannon.
Putting this into perspective makes it much easier to imagine why these dietary ‘guidelines’ may have been shaped by conflicts of interest.
Where to learn more about the US’s new dietary guidelines
I’ve spent the last several sections pulling apart the AHA’s guidelines. Now, I want to spend a moment talking about the newest US dietary guidelines.
It follows what I’d like to call a proper human diet: whole, real food, no added sugar, and high quantities of animal protein. And unlike the suggestions given to us by AHA, we have scientific evidence to suggest that the US dietary guidelines can help reduce poor cardiometabolic outcomes with:
To learn more about the benefits and application of this specific diet, I’d recommend starting with the following articles:
