Considering one in eight Americans now live with type 2 diabetes, it’s no surprise that more people are paying attention to their blood sugar.
Whether you’re diabetic or not, I imagine it’s also something on your mind. You’ve likely run into all sorts of research, tips, or suggestions for managing your blood sugar, like cutting sugar, avoiding fruit, or eating more eggs for breakfast.
But just like gut microbiomes and epigenetics, the way your body handles sugar won’t necessarily be the same as another person’s. At least, it’s more likely to fall in one of three categories.
Understanding how this works (and where you fall in the spectrum) can make a substantial difference in your metabolic health.
Here’s a quick overview to get you started:
- Glucotypes group patterns of blood sugar responses to help you better understand your level of blood sugar control.
- There are three different glucotypes: Glucotype L, Glucotype M, and Glucotype S.
- Knowing which glucotype you are can help you make better choices for your metabolic health, and potentially stave off heart conditions.
- You can use a CGM and an online tool to determine your glucotype.
- To improve your glucotype, you should focus on optimizing pillars like sleep, stress, exercise, low-carb eating patterns, and avoiding sugar.
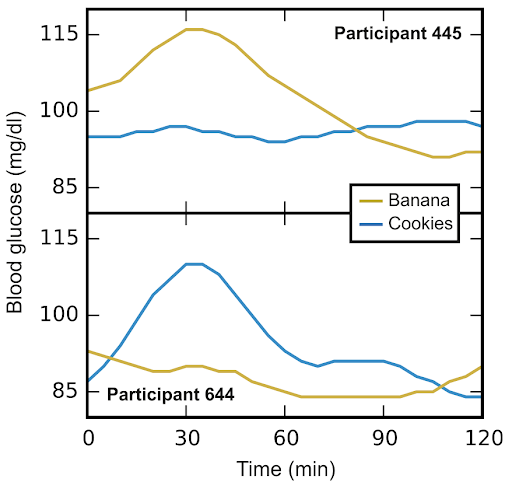
Source: https://x.com/nicknorwitz/status/1965128429734432943
Glucotypes are categories of blood sugar changes based on individual responses to food, exercise, or lifestyle choices. Or, as explained by the Public Library of Science, a “comprehensive measure of the pattern of glucose excursion.”
Take a look at the graph above depicting the glucose levels of two people. Both of these participants ate a cookie and a banana on separate occasions. But Participant 445 saw a dramatic change only after the banana. Participant 644, on the other hand, actually dropped their glucose level after eating the banana. They have an inverse response to the same exact foods.
The actual term ‘glucotype’ comes from a landmark 2018 study that used CGM data to track how much and how quickly a population’s blood sugar changes in response to food. Researchers collected a half-million glucose measurements from 57 participants (three of whom were diabetic, 14 prediabetic, and 40 normoglycemic responses).
The researchers found three distinct patterns, or glucotypes, among participants:
Glucotype L (Low Variability)
Type L was the most common glucotype among participants, at about two in five people studied. This was characterized by — you guessed it — low variability in spikes. Most individuals saw very low increases in blood sugar after meals, which remained relatively stable throughout the day.
Glucotype L was also associated with better metabolic health markers, such as lower values for:
- HbA1c
- Oral glucose tolerance tests (OGTT)
- Steady-state plasma glucose level (SSPG), or a test of insulin sensitivity
- BMI, aka likelihood for obesity
This, as you might imagine, is the most desirable glucotype for most people.
2. Glucotype M (Moderate Variability)
Moderate variability means exactly what you’d think: moderate glucose spikes that are easily predicted after meals. About 35% of those studied, or one in three people, fall into the Glucotype M category.
This is also the subgroup with the most opportunity for optimization. You might not necessarily be at risk for diabetes according to traditional tests, but you may want to keep an eye on your spike levels and frequency.
We’ll get into more specifics later on. But for now, keep in mind this is likely where most ‘healthy’ Americans sit.
3. Glucotype S (Severe Variability)
Roughly 25% of those studied experienced large, prolonged glucose spikes after meals. It could take hours before your glucose returns to baseline, even if you don’t feel any different from a functional standpoint.
Most people who experience large glucose fluctuations suffer from a comorbidity such as insulin resistance. They’re also typically glucose intolerant, meaning things that don’t normally affect roughly 75% of the population could severely affect their blood glucose (i.e., fruits like apples and mangos).
This is also the group that’s at the highest future risk for metabolic disorders, including diabetes, hyperinsulinemia, and heart attacks.
Why does it matter that we know our glucotype at all?
I’ll give you three major reasons:
- Glycemic variability (aka, blood sugar changes) is a very strong indicator of heart disease. Yet another reason why you should wear a CGM after a heart attack. As the glycotypes study itself points out: “recent evidence suggests that glycemic variability, more than fasting glycemia or HbA1c, predicts development of cardiovascular disease, possibly via oxidative damage causing endothelial dysfunction.”
- Your average one-off blood test may not capture the full picture of your metabolic health. Even people considered ‘normal’ by average reference ranges may have metabolic stressors and blood sugar spikes that point toward underlying dysfunction. This also means you can benefit from lifestyle changes at a much earlier stage, hopefully well before disease develops.
- Your glycemic subtype may help determine which foods are worsening your glycemic control. One study published in 2025 found that people who are less metabolically healthy respond differently to different food types (i.e., grapes and pasta). You may be able to identify conditions such as insulin resistance or beta-cell dysfunction long before experiencing chronic disease. This can also help you sculpt a more personalized nutrition plan rather than follow broad dietary guidelines.
How to identify your glucotype
The best and most efficient way to identify your glucotype is to wear a continuous glucose monitor. You’d be in very good company — there are an estimated 2.4 million people who have turned to CGMs to monitor their blood sugar response to food.
Track your response for a minimum of four weeks. Keep in mind the longer you track, the more valid your data will be.
Then, use this CGM viewer available online to determine your glucotype.
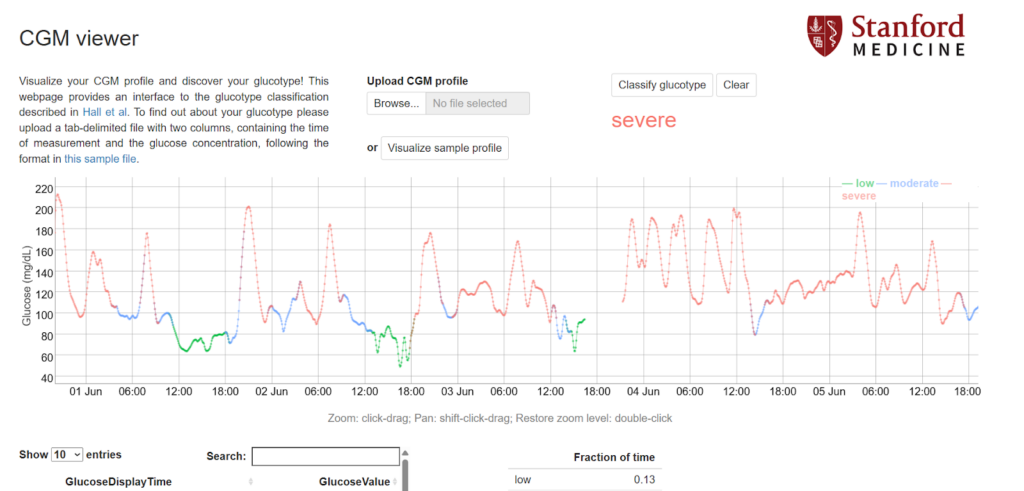
It’s true that wearable health tech isn’t an end-all-be-all for your health. It’s also not necessarily an infallible tool. But it can still give you a clue as to what you’re facing, and help you make more informed decisions about improving your metabolic health.
Improving your metabolic health based on your glucotype
No matter where you’re at with your metabolic health journey, there’s always room for some level of improvement.
This applies even if you’re in Glucotype L. Yes, your blood sugar spikes are mostly under control, but that doesn’t mean you can ignore sleep and stress management. Remember: these factors affect glucose even in otherwise ‘healthy’ people.
Glucotype M leaves plenty of room for optimization. Try looking for any personal trigger foods and temporarily moderating or cutting them out of your diet. You can also take a 10- to 15-minute walk after meals to help reduce your glucose spike. Apart from exercise, meal order can help. Some studies suggest eating carbs last can help blunt the impact of glucose spikes (although you should still eat carbs in moderation).
If you fall into Glucotype S, however, you’ll need to make significant lifestyle changes quickly. This will help you avoid the onset of chronic disease or other conditions that could impair your metabolic health.
For severe spikes, I recommend:
- Following a no or low-carb diet. Yes, this includes cutting sugar.
- Hydrate more. In some cases, this may include consuming more salt.
- Weight training. More muscle mass means better glucose management.
Perhaps most importantly, you need to work with a doctor who ‘gets’ it. If your primary provider can’t at least acknowledge the importance of bioindividuality, I would strongly suggest firing your doctor and looking for more holistic metabolic support.
If you’re searching for something like this, you’re welcome to speak with a member of my team.
